In the past two years, the Centers for Medicare & Medicaid Services (CMS) has been actively implementing and revising rules and regulations for previously established legislation that directly impacts Medicare payments related to Graduate Medical Education (GME). These actions will ultimately fix the existing payment penalty for hospitals that host fellowships and exceed full-time equivalent (FTE) training limits. On August 1, 2022, CMS issued the FY 2023 Hospital Inpatient Prospective Payment System (IPPS) Final Rule that changed the methodology used to reimburse hospitals that directly incur residents’ and fellows’ training costs and addresses the recent U.S. District Court opinion in Milton S. Hershey Medical Center, et al. v. Becerra.
On May 17, 2021, the U.S. District Court for the District of Columbia ruled in favor of the plaintiffs. The case, Milton S. Hershey Medical Center, et al. v. Becerra, argued that the methodology used to weight FTEs for direct GME payments was unlawful and misrepresented the regulation at 42 CFR 413.79(c)(2)(iii). What was known as the ‘Fellow Penalty’ reduced the weighting factor for hospitals training fellows from 0.50 to a lesser amount.
Background
Medicare direct GME payments are calculated by multiplying the hospital’s per resident amount (PRA) by the weighted number of resident FTEs and the hospital's Medicare days ratio. Section 1886(h)(4) of the Social Security Act set the methodology for determining the resident FTE counts for direct GME payments. This methodology is based on whether the resident has exceeded the initial residency period (IRP) or program length for board eligibility as set by the ACGME for that program. The resident “weighting factor” was applied beginning on or after July 1, 1987, and a resident that has exceeded their IRP is weighted at 0.50 of an FTE for Medicare direct GME payment. A resident training outside of their IRP is deemed a ‘fellow’ and a resident training in their IRP is weighted at 1.0.
Prior to 1997, both indirect and direct GME payments to hospitals were determined using the number of resident FTEs. As such, higher FTE counts resulted in higher payments. In response and to control Medicare’s spending on GME, Congress passed the Balanced Budget Act of 1997 (Pub. L. 105-33), which established a limit or cap on the number of allopathic and osteopathic residents a hospital could include in its resident FTE count for IME and direct GME payment. Dental and podiatry residents are not subject to this cap.
Resident FTE caps were established based on the FTE amounts reported in the most recent cost report period ending on or before December 31, 1996 and effective for cost reporting periods beginning on or after October 1, 1997. Hospitals that become teaching hospitals after 1996 establish a cap after the fifth program year. The resident FTE cap established under Section 1886(h)(4)(F) of the Act was based on a hospital’s unweighted FTE count. However, direct GME payment is based on the weighted FTE count. For that reason, CMS created a calculation to reduce the FTE amount so as not to exceed the cap, and account for fellows in the process. This calculation fundamentally reduced the direct GME payment for each hospital-trained fellow. When applied, it reduced the weighting factor for hospital’s training fellows from 0.50 of an FTE to a lesser amount, which became known as the ‘Fellow Penalty.’ See Exhibit A below illustrating how the described methodology impacted the weighted FTE amount used for payment.
Milton S. Hershey Medical Center, et al. v. Becerra
Milton S. Hershey Medical Center, et al. (the plaintiffs) argued that CMS’ proportional reduction method unlawfully reduced the weighting factor of 0.50 to an amount less than the 0.50, thus reducing the capped unweighted FTE amount to which hospitals are entitled for direct GME payment purposes. The court granted the plaintiff’s motion for summary judgment, denied the defendants, and remanded to the Agency so that it could recalculate the plaintiff’s reimbursement payments consistent with the court’s opinion. The court held that CMS’ proportional reduction methodology, enacted at 42 CFR 413.79(c)(2)(iii), was inconsistent with the statutory weighting factors and ordered the court to pay the plaintiffs using a more favorable method.
FY 2023 IPPS Final Rule
Because of the Court’s decision, CMS finalized its proposed policy and regulations text at 42 CFR 413.79(c)(2)(iii) to state that, effective for cost reporting periods beginning on or after October 1, 2001, “if the hospital’s unweighted number of FTE residents exceeds the cap described in this section of the final rule, and the number of weighted FTE residents in accordance with § 413.79(b) also exceeds that cap, the respective primary care and obstetrics and gynecology weighted FTE counts and other weighted FTE counts are adjusted to make the total weighted FTE count equal the limit.” If the number of FTE residents weighted in accordance with § 413.79(b) does not exceed that cap, then the allowable weighted FTE count is the actual weighted FTE count.1
- Effective for cost reporting periods beginning on or after October 1, 2001, this modified methodology will be used to determine the prior year’s weighted FTE count on Line 12 of Worksheet E 4, and for the purpose of determining the penultimate year’s weighted FTE count on Line 13 of Worksheet E 4; even though the prior and penultimate years’ FTE counts would be from cost reporting periods prior to October 1, 2001. For cost reporting periods beginning on or after October 1, 2001, the modified methodology would be fully applied to determining the direct GME payment.
- The new payment methodology will be applied to the MMA (Medicare Modernization Act of 2003) Section 422 FTE cap on Worksheet E-4 Line 20–24.
- CMS is also making a confirming change to regulations text at 42 CFR 413.79(d)(3) regarding application to the 3-year rolling average to state that “for cost reporting periods beginning on or after October 1, 2001, the hospital's weighted FTE counts for the preceding two cost reporting periods are calculated in accordance with the payment formula at 42 CFR 413.79(c)(2)(iii).”2
- CMS engaged in retroactive rulemaking to establish the rule effective for cost reporting periods beginning on or after October 1, 2001. According to 42 CFR § 1885(c)(2), any succeeding final rule applying the prospective new policy would not be cause to revisit final settled NPRs. CMS believes it would be inconsistent with the statute to calculate past payments for open cost reports based on a rule inconsistent with the law.
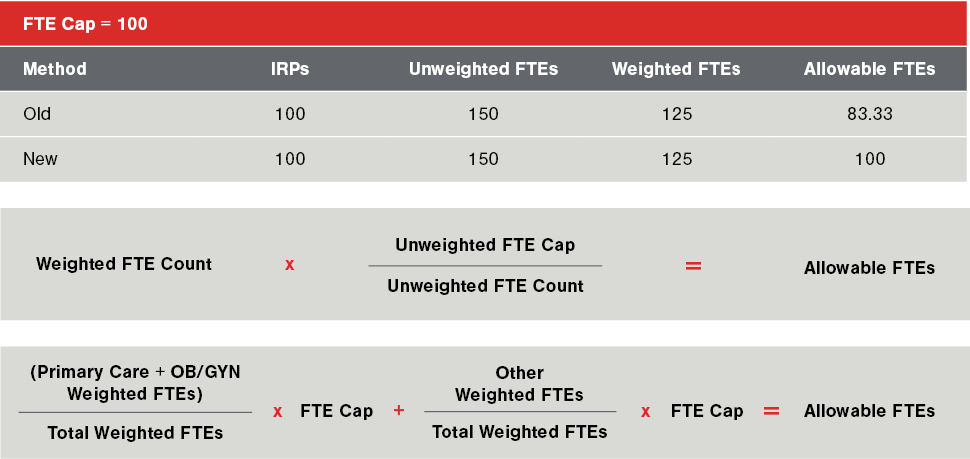
Exhibit A shows an example using the same scenario for a hospital with a resident FTE cap of 100. Under the old methodology, the hospital’s weighted FTEs for direct GME payment would be 16.67 less than under the new methodology. In this example, the hospital’s unweighted and weighted FTE counts are over its cap. However, the hospital is now held harmless at its resident FTE cap. This difference can result in millions of Medicare reimbursement dollars, depending on each hospital’s situation. It could also result in additional Medicaid payments for hospitals in states that follow the Medicare methodology.
Exhibit A
Next Steps
FORVIS will provide guidance as your organization responds to the Court’s decision and subsequent CMS changes to rules, regulations, and reporting. Our current understanding is that each MAC will automatically apply the new methodology to open cost reports with some MACs already issuing correspondence to plaintiffs notifying them of pending cost report updates. We recommend organizations work with the Healthcare Consulting Reimbursement Team at FORVIS to decide whether MAC is appropriately updating all applicable cost reports. We anticipate CMS will issue a transmittal soon outlining the appropriate Medicare cost report changes and shortly after that HFS will update the cost report software.
In the interim, we recommend organizations perform the following:
- Identify all open cost report years not yet settled by the MAC
- Identify all open cost report years amended for an issue specific to a direct GME
- Identify all NPR cost report years with the DGME penalty as a protested item
- Identify NPR cost reports still within the 180-day appeal window if DGME penalty is not included as a protested item
- Discuss the cost report treatment for June 30, 2022 year-end providers impacted by the ruling and methodology changes
- Calculate the Medicare reimbursement impact and make appropriate changes in due to/from amounts
The revised calculation does not reduce weighted FTEs below the cap. Under the old methodology, only the hospital’s unweighted allopathic and osteopathic FTE count was compared to its FTE cap if they exceeded the FTE cap. The new methodology has an additional step to compare the weighted allopathic and osteopathic FTE count to the FTE cap.
Reach out to the Healthcare Consulting Reimbursement Team at FORVIS or submit the Contact Us form below if you have questions.

